Actinic Keratosis & Precancerous Growths
The term “precancerous” is used because these abnormal areas of skin are more likely to turn malignant than healthy skin. Precancerous growths (lesions) are visible to the naked eye, and they look different from normal cells when examined under a microscope. They are important to recognize, because they are a warning sign of potential skin cancer.
Actinic keratoses (AKs) are rough, dry and scaly patches of skin that develop on the outermost layer of the skin after years of exposure to ultraviolet (UV) rays of the sun. Often they feel like sandpaper or crusts of dry skin. These lesions typically range in color from skin-toned to reddish brown and in size from that of a pinhead to larger than a quarter. Occasionally, a lesion has a rapid upward growth and resembles an animal horn and is called a “cutaneous horn.”
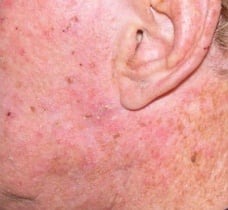
A dermatologist should evaluate anyone who is suspicious that may have developed AKs. These lesions are considered to be the earliest stage in the development of skin cancer and can progress to squamous cell carcinoma, a type of skin cancer that can be fatal. Having AKs makes one more susceptible to other forms of skin cancer, including melanoma. Melanoma is considered the most lethal form of skin cancer because it can rapidly spread to the lymph system and internal organs.
AKs are most likely to appear on the face, lips, ears, scalp, neck, backs of the hands and forearms, shoulders and back — the parts of the body most often exposed to sunshine.
AKs usually appear after age 40 because they take years to develop. However, even teens can have AKs when they live in areas that receive high-intensity sunlight year round, such as Florida and Southern California.
Millions of Americans have AKs, and the number continues to grow. In fact, AKs are so common today that treatment for these lesions ranks as one of the most frequent reasons people consult a dermatologist.
Treatment Options for Actinic Keratoses
There are three main categories of treatment for actinic keratoses.
- Destructive treatments. Most commonly, individual actinic keratoses are frozen or “burned” off with liquid nitrogen. This eliminates that focus of abnormally growing cells. Occasionally, the disorganized layer of cells can be electrodesiccated with an instrument called a hyfrecator, or removed with an ablative laser. Thick lesions, more common on the scalp and extremities can be scraped away under local anesthesia with a curette. Regardless of the treatment, only the visible actinic keratoses are treated with these methods, and damaged cells not visible to the naked eye soon develop into new actinic keratoses.
- Topical chemotherapy creams and immune response modifiers. Topical chemotherapy creams (Efudex, Carac) most commonly contain 5-FU, a fake DNA building block that is incorporated into rapidly dividing cells and leads to their destruction. Imiquimod works by stimulating the immune system to recognize the presence of these abnormal actinic keratoses cells, and the immune system eliminates them. Both of these treatments have the advantage of treating subclinical lesions–abnormal skin cells that have not yet developed into visible actinic keratoses.
- Photodynamic Therapy (PDT). Photodynamic Therapy uses a combination of a photosensitizing medicine and visible light to destroy the precancerous cells. A medication, Levulan, contains a by-product of red blood cells called porphyrin. Porphyrins naturally cause an intense destructive reaction in cells that lack an enzyme to break them down metabolically. It turns out that precancerous actinic keratoses lack the enzyme to metabolize porphyrins. These cells absorb the medication when it is applied to the skin, but they are simply not able to clear it like normal cells. Consequently, when the skin is exposed to visible blue light the abnormal cells are targeted and are eliminated. PDT also is capable of treating invisible (subclinical) damage as well. This results in typically a longer period of clearance of actinic keratoses in a treated area.